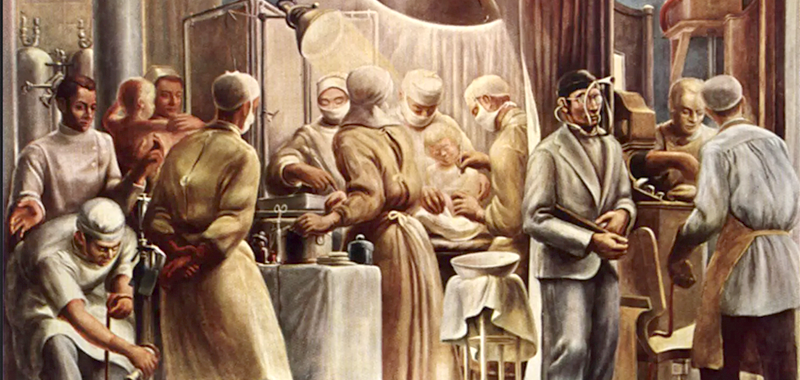
“There is no reason for the surgeon to learn on the patient”. This sounds like a recent saying from one of the last conferences we visited! Guess when Dr. Will Mayo has said this very true words? It was in 1929…
Unfortunately, almost 100 years later, we are still discussing the pros and cons of medical simulation. An implementation across a broader basis of specialties and countries around the world seems still far away.
Still, we keep hearing from our colleagues, hospital managers and other healthcare providers excuses like “oh this technology is so new, we have not had time to look on it”. “This must be a new thing from the US”, some add. Unfortunately, both statements are somehow incorrect. Medical simulation and medical simulators are far from being “a brand-new development”.
But when did the idea of simulation in healthcare came up?
We know today, thousands of years ago, certain models were already used to help teach anatomy and physiology.
The earliest simulators in the history of medicine that are somehow like those we know nowadays were the obstetrical manikins introduced towards 1700 by family Grégoire in France. They were meant to teach midwives and could leak blood and amniotic fluid.
Some years later the “epicenter of medical simulation” moved from France to Italy. In the 19th century, the movement of clinical simulation was more located in the UK, France and Germany.
This shows, manikins and simulators have at least a history of 250 years and are not really “a new thing” in the education of healthcare professionals.
What is somehow true that until a couple of years ago this technology was not well used or established on a broader basis [J B Cooper, V R Taqueti, A brief history of the development of mannequin simulators for clinical education and training, Qual Saf Health Care 2004;13(Suppl 1):i11–i18. doi: 10.1136/qshc.2004.009886].
It took until the 1960s when simulators were more and more used for the training of doctors, nurses, and laymen in resuscitation techniques [Buck GH. Development of simulators in medical education. Gesnerus. 1991;48 Pt 1:7-28. PMID: 1855669.]. Responsible for this development was a “simulator” called Resusci-Anne. This mannequin for training in mouth-to-mouth ventilation was designed by Asmund Laerdal, a Norwegian manufacturer that is well known nowadays.
A couple of years later (1968) a product called “Harvey” appeared on the market. It is a full-sized mannequin that simulated almost 30 cardiac conditions by then. It is one of the first examples of the modern concept of a task trainer made for medical skills training. It has undergone a rigorous testing for educational efficacy, perhaps more than any other simulation technology so far out there.
Due to the success of “Resusci-Anne”, the Laerdal company developed a higher fidelity mannequin, but not before the mid-1990s. The product was called “SimMan”.
Also, in the mid-1990s, David Gaba reported a broader and year-long use of medical simulators especially in the field of anesthesia as well as a 10 year experience in using simulation for crisis / crew resource management trainings [Gaba DM. Simulators in anesthesiology. Adv Anesth 1997;14:55–94. ; Gaba DM, Howard SK, Fish K, et al. Simulation-based training in anesthesia crisis resource management. (ACRM): a decade of experience. Simulation Gaming 2001;32:175–93].
At the turn of the century, more and more lifelike manikins, task trainers and others appeared across more and more specialties, and it became obvious that they are an important training modality not just in undergraduate but also in postgraduate medical and nursing education.
It helped to show that aviation did the same for their crews, being most often cited as the example to follow. That experience has influenced the development of medical simulators for sure a lot.
I guess one can say that the turn of the century was one of the breakthrough points of the medical simulation movement.
Some years later (2008), in a study by Okuda [Okuda, Bond: National Growth in Simulation Training within Emergency Medicine Residency Programs, 2003–2008] it was published that already 91% of residency programs in Emergency Medicine in the US use some form of simulation as training possibility. 85% of programs specifically use mannequin-simulators, compared to 29% 5 years earlier. 43% of the programs reported that – in 2008 – annual resident simulation use by then averages more than 10 hours per year.
This increase in usage of simulation is another important point that shows, how fast the idea of simulation was implemented in some areas.
That more and more specialties use simulators and modern technology now to train their students, residents and other healthcare providers is followed by the development of more and more simulators for healthcare.
“There is no reason for the surgeon to learn on the patient” is a citation from almost 100 years ago. Let’s make sure it is not taking another 100 years until this idea is fully implemented in healthcare education and accessible to all learners.
Written by Lukas Drabauer from Alpha Medical Concepts (AMC)