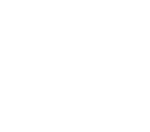
The simulation teaching approach requires more time, resources and preparation than the traditional method.
Despite this slower pace, the simulation-teaching method guarantees an immediate increase in the knowledge acquired and greater confidence in what has been learned.
The study shows this: “Li CH, Kuan WS, Mahadevan M, Daniel-Underwood L, Chiu TF, Nguyen HB; ATLAS Investigators (Asia neTwork to reguLAte Sepsis care). A multinational randomised study comparing didactic lectures with case scenarios in a severe sepsis medical simulation course. Emerg Med J. 2012 Jul;29(7):559-64″ demonstrated that Medical simulation adds value to a lecture-only course by increasing the knowledge of emergency physicians’ management of SEPSI in the emergency department.
The study aims to understand the effect of the standard lessons compared to the simulated scenario on cognitive knowledge and skills.
This prospective randomised study enrolled 98 Emergency doctors at all levels of training from four centres in Taiwan, India and Singapore. All participants received a 5-hour course that included teaching lessons, workshops and a clinical case scenario based on sepsis.
The participants were randomised in two arms: 1) before the theoretical lesson and 2) before the simulation. All the centres used a high-fidelity adult patient simulator (SimMan, Laerdal Medical, Stavanger, Norway) and dummy torsos for central venous catheter insertion and endotracheal intubation. The workshop and scenario were both considered the simulation part of the course.
Participants were given an assessment test of 20 questions: before the course (pre-test), after completing the first part of the course (post-test 1) and at the end of the course (post-test 2).
A checklist that contains 21 items considered critical for targeted early therapy and resuscitation of septic shock evaluated the achievement of the objectives in the simulation.
Overall there was a significant progressive improvement in test scores for all participants (p <0.01). The pre-test scores were similar in the two groups. The first group (before the lesson) had a score significantly higher in post-test one than the group doing the simulation before. However, the post-test 2 score was similar for both groups at the end of the course.
Participants had a significant improvement in confidence level at the end of the course in managing patients with severe sepsis and septic shock (p <0.01).
The group that did the lesson earlier was faster in assessing the lactate level and identifying the need for saturation and central pressure monitoring.
Central venous catheter insertion and hemodynamic monitoring are also crucial for treating patients with septic shock who commonly require fluids and vasopressors. These skills are learned faster when performed in simulation.
The fact that these elements were achieved more often when participants had a teaching lesson before the simulated scenario suggests that participants, through a training model that includes both traditional teaching and simulation, best receive the concepts for timely management of severe sepsis and Septic shock.
The authors of this study conclude that a traditional course followed by high-fidelity simulation sessions on the management of severe sepsis and septic shock, focusing on the team approach, should be commonplace in emergency medicine training to achieve an immediate increase in knowledge in the management of sepsis.
Therefore, thanks to the combination of medical simulation with teaching lessons, this method could also prove valuable in analysing the leading causes of sentinel events and improving protocols and guidelines.
Written by Francesco Barberio & Roberta Caporusso