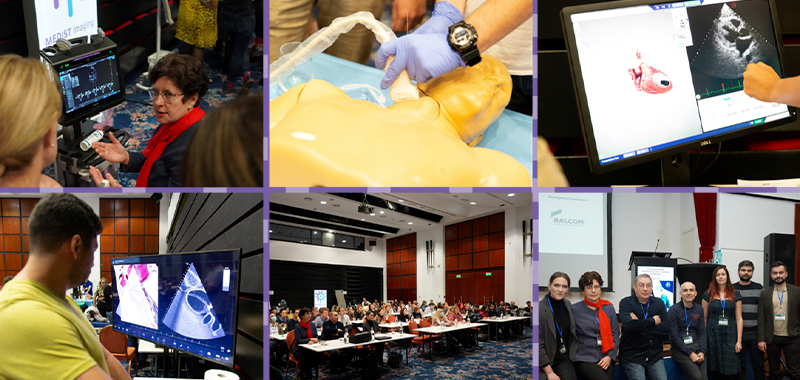
CESIMUS, a pioneer in simulation-based teaching of critically ill ultrasonography. Lower right corner, CESIMUS team (order from left to right): Dr. Bianca Morosanu, Dr. Ioana Marinica, Prof. Dr. Serban I. Bubenek-Turconi, Dr. Cosmin Balan, Dr. Liana Valeanu, Dr. Cornel Robu, Dr. Mihai Stefan.
Simulation continues to become more entrenched and refined in all aspects of medical training. Traditionally, simulation has provided a coherent, risk-free platform to hone the skills and inculcate the cognitive and interpersonal behaviors that drive optimal team performance. Nevertheless, the recent adoption of simulation to teach ultrasound (US), mechanical ventilation, hemodynamics, and extracorporeal life support reflects a paradigm shift towards a holistic, more integrated approach focusing on applied physiology which has always been the foundation of intensive care medicine.
Critical care ultrasound (CCUS) is ubiquitous in modern-day clinical practice, providing answers to questions meant to deploy real-time personalized therapeutic support. Furthermore, US guidance was demonstrated to boost safety during vascular cannulations and even spark intensivists’ interest in procedures otherwise prohibitive outside surgical competence. The latest CCUS consensus statement precisely delineated the basic US skills and competencies in the intensive care settings[1]. However, it did not determine the best way to achieve these within a formal training program. As hinted above, worldwide cumulating evidence, mostly of anecdotal origin, suggests that simulation may play an essential role. CESIMAB (Centre of Simulation in Anesthesia and Intensive Care Medicine Bucharest) provides a similar testimony. For the past three years, our group has been running successfully CESIMUS, a national workshop of critically ill ultrasonography mainly directed at anesthetists and intensivists. CESIMUS includes three core competencies (i.e., cardiac, lung, and vascular cannulation) within a mixed educational program consisting of lectern and interactive lectures and hands-on sessions on healthy volunteers and high-fidelity mannequins. CESIMUS paved the way for a national simulation-based attestation program in CCUS starting in late 2023.
Recently, CESIMAB explored the utility of simulation within an educational program that integrates protective mechanical ventilation and hemodynamics. Again, feedback was more than promising. Mechanical ventilation with a hemodynamic nutshell is the epitome of applied physiology benefiting from simulation. We are familiar with the mantra, “just because we can, doesn’t mean we should.” As a case in point, this is particularly true with the undifferentiated use of higher positive end-expiratory pressures and recruiting maneuvers which were shown to be deleterious. However, this mantra no longer holds if under a simulation-based protective environment. Trainees are then free to test and cross the limits of physiology to answer their most arduous questions. CESIMAB trains with the ASL 5000TM (IngMar Medical, 5940 Baum Blvd. Pittsburgh, PA 15206 USA) and LungSimTM (Gaumard, Gaumard Scientific, Canada). These high-end simulators present a complete lung solution that can emulate the entire range of human mechanical time constants and beyond. CESIMAB is committed to ingraining simulation in its upcoming ECLS workshops.
To conclude, it would be wise to consider that the best way to predict time is staying ahead of time. Education-wise, how we train will continue to evolve and revolve around simulation. Therefore, you should choose simulation early and extensively regardless of your domain, but all the more reason if you practice anesthesiology or intensive care.
Written by Dr. Cosmin Balan, Dr. Mihai Stefan, Dr. Liana Valeanu, Dr. Cornelia Predoi, Dr. Cornel Robu, Dr. Ioana Marinica, Dr. Bianca Morosanu, Prof. Dr. Serban I. Bubenek-Turconi, Prof. Dr. Daniela Filipescu
[1] C. Robba et al., “Basic ultrasound head-to-toe skills for intensivists in the general and neuro intensive care unit population: consensus and expert recommendations of the European Society of Intensive Care Medicine,” Intensive Care Med., vol. 47, no. 12, pp. 1347–1367, Dec. 2021, doi: 10.1007/s00134-021-06486-z.