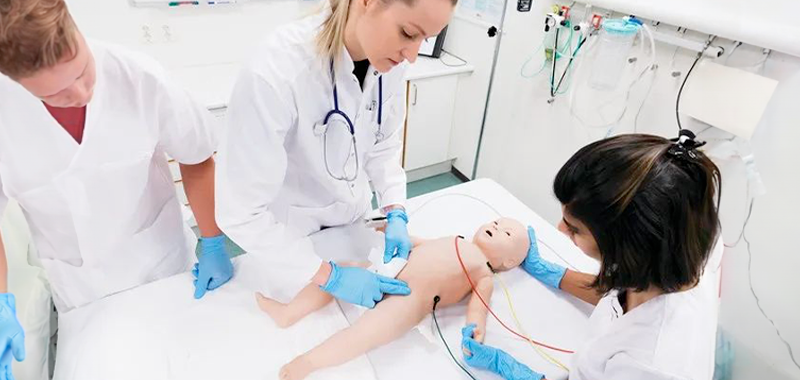
Simulation in neonatology is of great help in improving and maintaining skills in dealing with rarely occurring situations such as neonatal asphyxia, which, however, require rapid intervention. During the pandemic, we analyzed whether the personal protective devices necessarily worn in the case of delivery by a COVID-positive mother could also be an obstacle to the resuscitation of an asphyxiated neonate.
This study involved neonatal intensive care units in Bolzano and Padua. It was published in the Archives of Disease in Childhood Fetal and Neonatal Edition (Impact of personal protective equipment on neonatal resuscitation procedures: a randomized, cross-over, simulation study; Francesco Cavallin, Fiorenzo Lupi, BenedettaBua, Marion Bellutti, Alex Staffler, Daniele Trevisanuto).
Specifically, by performing neonatal resuscitation simulations on a manikin, we compared the timing of resuscitation interventions at birth, comparing conditions requiring personal protective equipment(PPE) and standard conditions without wearing PPE in a simulation scenario.
We also assessed participants’ perceptions of discomfort using PPE and its impact on resuscitative procedures by administering a questionnaire.
The study involved 12 teams divided into two groups: one facing a standard resuscitation scenario and the other, remotely, a scenario involving the resuscitation of the newborn child of a COVID-19-positive mother. From the call to birth, the participants had 2 minutes for preparation. After that, we assessed the time when resuscitation was started, the time required for intubation, and the appropriateness of using PPE.
The participants were then administered a questionnaire asking whether they had experienced more difficulty with movement, visual challenges, temperature discomfort, or communication with the use of PPE.
The results showed that the use of PPE worsened the performance of the teams. In particular, there was a time delay until the initiation of resuscitation and also until intubation. However, all teams still managed to initiate ventilation within 1 minute of life (as per guidelines).In addition, only 25% of the teams intubated the infant before starting chest compressions, and 70% of the teams did not start the timer for Apgar at the infant’s birth. Regarding the use of PPE, the tight schedule facilitated errors such as not fastening the gown before entering the contaminated area or wearing the headset incorrectly.
Wearing PPE was subjectively associated with visual limitations, discomfort in movements, limitations in communication and thermal discomfort.
Written by SABES team, Italy