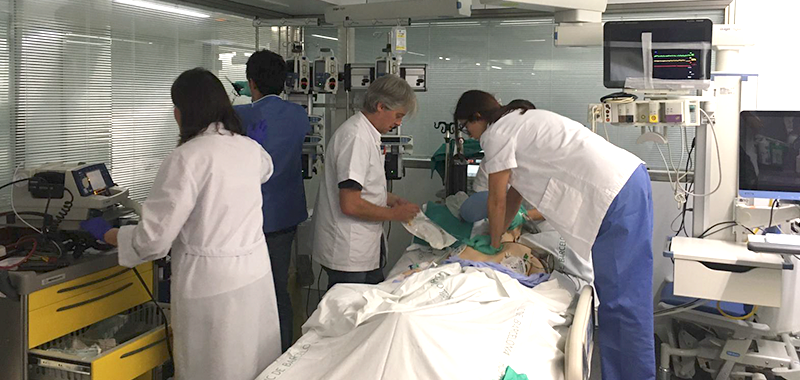
Clinical simulation (CS) is a very useful tool to bridge the gap between theoretical knowledge and real practice. It allows training professional skills in a safe environment for patients and also for professionals.
The first time we heard about CS, we imagined large specialised centres with complex, highly technological environments, where quasi-human mannequins allow recreating experiences that are close to reality without affecting the patient. But then, is it only possible to do CS in these places? Absolutely not. Here we show you some ideas:
It is true that having a place to carry out the activity is a necessity, and generally, a minimum of specific material is also required. When it is not possible to use specific facilities for CS in our centre, in situ simulation can be carried out, which also increases fidelity and encourages the participant to focus on the clinical problem instead of on the environment, since it is familiar to them. With in situ simulation, there is no need to use props. The clinical material used for the simulation may come from expired or not-suitable-for-medical-use assets. Nevertheless, to avoid potential problems in in situ simulation it is necessary to mark all the simulation material and check the real material used to replace it at the end of the session. It is also convenient to notify all the personnel of the chosen location that a simulation is being carried out and also make sure that they know the emergency signal used to stop the simulation in case a real problem happens.
Regarding specific simulation material, basic monitoring (numerous low-cost applications are available), a low-medium fidelity mannequin, or specific phantoms for techniques placed on a simulated patient are often enough. In this type of scenario, the interaction between patient and professional increases the perception of fidelity.
So far, we have only talked about where and how. However, in CS the most important things are what, to whom and by whom. In other words, a well-trained team of facilitators that know how to identify the needs of the participants and create an activity that gives rise to deep reflection during the debriefing is more important than materials and technology. The SAFETY team is working on identifying these needs in our future professionals, and offering them a specifically-designed program that can help colleagues from any European institution to carry out CS activities.
Large simulation centres have an irreplaceable role; nevertheless, low-cost simulation is possible, since CS is not synonymous with technology, but rather a tool the results of which depend on the team behind it.
- https://www.inacsl.org/healthcare-simulation-standards
- Shrestha R, Shrestha AP, Shrestha SK, Basnet S, Pradhan A. Interdisciplinary in situ simulation-based medical education in the emergency department of a teaching hospital in Nepal. Int J Emerg Med. 2019 Aug 27;12(1):19. doi: 10.1186/s12245-019-0235-x. PMID: 31455223; PMCID: PMC6712774.
- Goldshtein D., Krensky C., Doshi S., et al. (2020). In Situ Simulation and its Effects on Patient Outcomes: A Systematic Review. BMJ Simulation and Technology Enhanced Learning, 6(1), 3-9. https://doi.org/10.1136/bmjstel2018-000387
- Chima AM, Koka R, Lee B, Tran T, Ogbuagu OU, Nelson-Williams H, Rosen M, Koroma M, Sampson JB. Medical Simulation as a Vital Adjunct to Identifying Clinical Life-Threatening Gaps in Austere Environments. J Natl Med Assoc. 2018 Apr;110(2):117-123. doi: 10.1016/j.jnma.2017.12.003. Epub 2018 Feb 15. PMID: 29580444.
Written by the Barcelona Team from Hospital Clinic for SAFETY Project